
What diseases are caused by the bacterium Staphylococcus aureus?
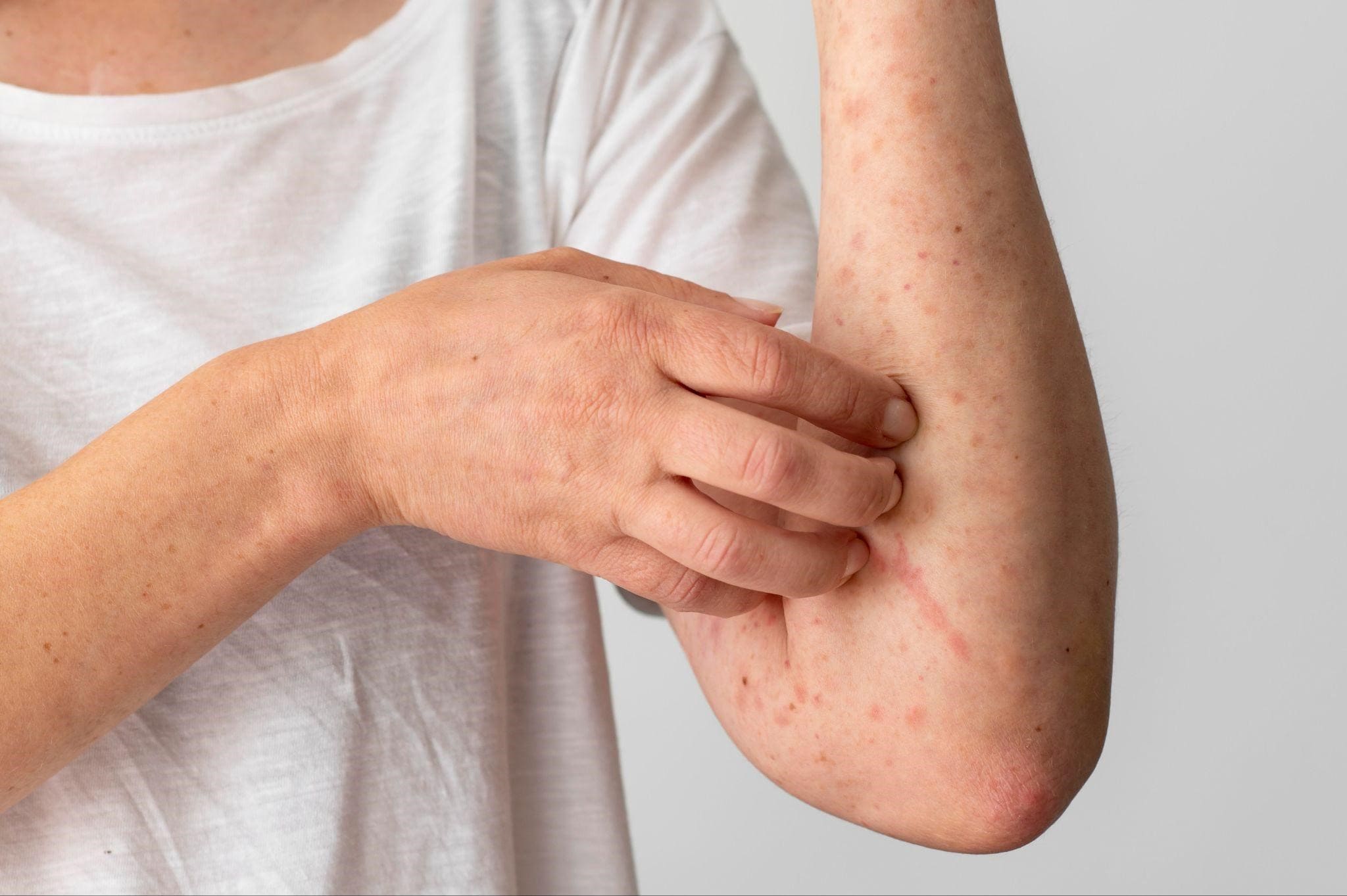
Skin diseases caused by bacterial infections are among the most common health problems affecting both children and adults. The most dominant bacterial pathogen infecting human skin is Staphylococcus aureus, even though this bacterium is also naturally found on our skin under normal conditions.
S. aureus can transform into an invasive pathogen when certain skin conditions allow its bacterial population to increase beyond normal levels. The uniqueness of this bacterium lies in its ability to produce various toxins, such as Panton-Valentine leukocidin (PVL), exfoliatins, enterotoxins, and toxic shock syndrome toxin-1 (TSST-1).
These toxins can cause mild localized infections such as impetigo and folliculitis, as well as severe conditions such as toxic shock syndrome and staphylococcal scalded skin syndrome. In the past decade, a serious condition that has become a major challenge in disease control has emerged, namely community-acquired methicillin-resistant Staphylococcus aureus (CA-MRSA).
Therefore, a comprehensive understanding of skin diseases caused by S. aureus and their pathogenic mechanisms is essential to support accurate diagnosis, effective treatment, and appropriate prevention.
- Why S. aureus Can Colonize the Skin?
- Interaction with Skin Microbiota
- Types of Skin Infections Caused by S. aureus
- Prevention Strategies
Why S. aureus Can Colonize the Skin?
S. aureus possesses unique biological adaptation mechanisms that allow it to survive, adhere to, and interact with the skin environment. In fact, human skin presents a hostile environment for bacteria due to its relatively acidic pH, dry and salt-rich surface, and the presence of fatty acids, antimicrobial peptides, and innate immune defenses.
However, due to its specialized adaptive mechanisms, S. aureus is able to persist and colonize the skin. One of these mechanisms is the production of adhesin proteins that enable the bacterium to attach to skin cells or surface tissues.
When this attachment is sufficiently strong, the bacteria can remain on the skin despite friction or washing. In addition, S. aureus has a high tolerance to salt, making it well adapted to human sweat.
Interaction with Skin Microbiota
Human skin is inhabited by normal microbiota such as Staphylococcus epidermidis and Cutibacterium acnes, which inhibit the growth of pathogenic bacteria (including S. aureus) under balanced skin conditions. However, when the balance of the skin microbiota is disrupted—due to antibiotic use, wounds, dermatitis, or excessive moisture—S. aureus can become dominant on the skin.
Colonization of S. aureus is commonly found in the nasal cavity, armpits and skin folds, the groin area, and on damaged or inflamed skin. Colonization can progress to infection when there is a break in the skin barrier, weakened immune defenses, and increased production of virulence factors and toxins by the bacterium.
Types of Skin Infections Caused by S. aureus
Localized skin infections caused by S. aureus include impetigo, which commonly affects children and is characterized by fragile blisters, pustules, and yellowish crusts. This infection is caused by exfoliative toxins A and B produced by the bacteria, which damage structural proteins in the skin, leading to separation of the epidermal layers.
Another common infection is folliculitis, which affects hair follicles and is accompanied by surrounding erythema. This infection occurs in hair-bearing areas of the body and is frequently found in the beard area as a result of shaving activities.
More severe infections are caused by bacterial toxins, such as toxic shock syndrome (TSS), which is induced by staphylococcal enterotoxins. The characteristic symptom is diffuse skin erythema resembling sunburn.
In addition, staphylococcal scarlet fever is also caused by enterotoxins. Systemic dissemination of exfoliative toxins can lead to staphylococcal scalded skin syndrome (SSSS), which is characterized by widespread blistering and a burned-skin appearance and most commonly affects young children.
Prevention Strategies
Prevention of skin diseases caused by Staphylococcus aureus focuses on maintaining skin moisture to preserve a healthy skin barrier. Good hygiene practices are essential, including regular bathing, especially after sweating, avoiding the sharing of towels, clothing, or razors, and maintaining cleanliness in skin fold areas such as the armpits and groin, which are preferred sites for S. aureus colonization.
Read this too:
Differences in Antimicrobial Testing Techniques: Classical and Modern Methods
Skin infections caused by Staphylococcus aureus not only affect individual health but can also pose serious risks in families, schools, healthcare facilities, and even industrial environments. When colonization progresses into infection, prompt and evidence, based management becomes essential to prevent complications and wider transmission.
Therefore, accurate bacterial identification and reliable laboratory testing are crucial to ensure that treatment and prevention strategies are truly effective. IML Testing and Research is ready to support you through microbiological testing services, pathogenic bacterial identification, and standardized antibiotic susceptibility testing.
With comprehensive analytical methods and dependable results, we help you make data-driven decisions for more effective infection control. Consult your testing needs with IML Testing and Research today.
Author: Safira
Editor: Sabilla Reza
Reference:
Del Giudice, P. (2020). Skin infections caused by Staphylococcus aureus. Acta Dermato-Venereologica, 100(9).



